

|
 |
| Causes of Conjunctivitis | Types of Conjunctivitis | Symptoms of Conjunctivitis | Allergic Conjunctivitis | Viral Conjunctivitis | Bacterial Conjunctivitis | Giant Papillary Conjunctivitis |
|
1. What is conjunctivitis? |
|
4. Is conjunctivitis contagious?
|
||
|
7. What are the problems of conjunctivitis in babies?
|
|
10. How can I prevent conjunctivitis? To keep from getting conjunctivitis from someone who has it, or to keep from spreading it to others, follow these guidelines:
Avoid close contact with people until you have used the antibiotics for 24 hours and if your eye does not have a lot of pus. Children can return to school or day care after they have had 24 hours of antibiotic treatment.
Vision is rarely affected. Infectious conjunctivitis can be distinguished from the allergic type with a thorough examination.
|
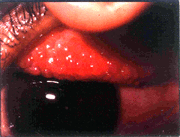 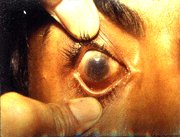
|
|
13. What are the common allergens that cause allergic conjunctivitis? Common allergens that cause allergic conjunctivitis include:
14. What are the types of allergic conjunctivitis? |
|
|
19. How long will the effects last?
22. What is bacterial conjunctivitis? |
Bacterial Conjunctivitis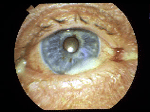 |
|
23. What organisms are commonly involved in bacterial conjunctivitis? Bacteria that commonly influence bacterial conjunctivitis are:
25. How long will the effects of bacterial conjunctivitis last?
|
|
|
30. What are the symptoms of GPC? Most often, the symptoms of GPC occur while the contact lenses are in place; however, they may persist after removal of the lens from the eye.
The symptoms described above may not necessarily mean that you have giant papillary conjunctivitis. However, if you experience one or more of these symptoms, contact your eye doctor for a complete exam.
31. What are the treatments for GPC?
|
|